FAQ
You Ask, We Answer
Dummy
Did you know?
- Physiotherapists work with people of all ages to bring about improvements in their health and independence.
- Studies have indicated that physical therapy treatments have a major impact on conditions such as back and neck pain.
- Physiotherapists provide exercise programs for conditions that affect the bones and muscles, such as arthritis, back and neck pain, osteoporosis, joint replacements, and urinary incontinence.
- Physiotherapists provide exercise prescriptions to help people keep fit and achieve/maintain a healthy weight.
- Around 350 million people are obese worldwide. Physical activity is one of the best means of countering obesity.
- Children and young people under the age of 18 need 60 minutes of moderate to vigorous physical activity each day to promote and maintain health.
- Adults need 30 minutes of moderate physical activity 5 days a week, or 20 minutes of vigorous physical activity 3 days a week to maintain health. Plus, they need to do muscle-strengthening exercises at least twice a week.
- Research has shown that physio exercise prescriptions help women who experience incontinence, suffer from osteoporosis or are recovering from breast cancer surgery.
- Physical activity provided under the guidance and supervision of a physical therapist reduces the risk of heart attack, stroke, type 2 diabetes, colon cancer, and breast cancer.
- If exercise was a pill, we would all be on it!
What to expect?
We always start with the same procedure: talking. We allow plenty of time for you to describe your symptoms or performance goals, allowing us in turn time to listen and thoroughly assess you before progressing. We believe the more time we take at the initial stage the more effective we can be in helping you to reach your goals faster and easier. We have the same approach for every client:
- Assessment
- Diagnosis
- Treatment Plan
- Result
What should I wear?
A degree of undressing may be required during the examination. Your physiotherapist will discuss this with you at the time. You should plan to wear suitable clothing: for example, we recommend wearing shorts if you have a leg or back injury. We also suggest that ladies wear a vest top for neck/shoulder injuries.
If you are attending our Sports Clinic is best to bring your usual sporting clothing and trainers.
Please refer to our update COVID -19 procedures for peace of mind.
Do you do Home Visits?
Regrettably no, we are busy in the clinic but will happily recommend some of our trusted physiotherapy colleagues to come at see you instead. They are happy to see you in your home until you are well enough to be able to come into the clinic to see us. Please call us for further information.
We recommend:
Sue Marks 07797740798
Dummy
Must I see my GP before booking a physio Appointment?
No, we do not require you to see your GP first. However, if you are privately medically insured, it is possible that your insurer may require you to see your GP, some may require you have a written referral from your GP.
Each of the insurers has different requirements so please do check your policy. If you have relevant results of tests or scans, please do bring them along to your physio appointment. If you feel they are relevant to your current injury, and you do not have copies, you could ask your GP to forward them to us in advance of your appointment with us.
We appreciate that sometimes there can be a blurred clinical picture and sometimes it is relevant to be assessed by your GP to help rule out non orthopaedic issues.
Why should I see my GP or an MSK/Sports Consultant or Orthopaedic Surgeon?
Your GP will be your first port of call for a broad range of medical ailments. They have a wide breadth of knowledge across all the specialities of medicine. GPs are not permitted to order MRI scans. An MSK or Sports Medicine Consultant will have additional specific qualifications in Sports Medicine. They are likely to be able to perform Ultrasound scans and order MRI scans of all body parts.
They can perform specific injections when relevant. An Orthopaedic Surgeon is quite specialised in their area. They are the experts in surgery. Physios work closely with all three Doctors; from the formulation of the diagnosis to delivering the rehab post-injection or postoperative.
How do you know your treatment is working?
Very simply, you will begin to feel better. You may find that you can sleep better, move better, feel less pain, or perform better. Objectively, when we examine you, we may find that you have greater movement, test stronger, have improved balance or jump higher.
Will my Physio give me homework to complete?
Yes, it is quite likely that we will. Through our vast experience and the scientific literature, we know that our bodies really benefit from doing specific movements at specific intervals. Your recovery is likely to be quicker and more complete if you follow the prescribed programme that we devise just for you. The right exercise, at the right time, the right number of sets and repetitions can make the world of difference.
Your exercises may be given to you in writing, or we may take a video of you on your phone so that you have an easy reference. Whatever works best for you, we will use that.
Am I supposed to “feel” it when I do my exercises?
Yes, we prescribe exercises for lots of different reasons. Some exercises are designed to move joints, sometimes it is to stretch a tight muscle, to retrain balance, strengthen muscles, mobilise nerves or retrain certain movement patterns.
It is rare that we would ever prescribe an exercise that would cause too much pain. If it does, please do let us know. Having an increased discomfort that is felt temporarily afterwards is completely normal.
How to register and book your 1st appointment
First time using our online booking system? Follow these simple steps and get your physiotherapy appointment booked online today!
How to book your first online appointment & register:
First time using our online booking system? Follow these simple steps and get your physiotherapy appointment booked online today!
1. Use the following link to access our online booking system: https://physiojersey.connect.tm3app.com/
2. Select ‘book an appointment’ and then select ‘physiotherapy’.
![]()
3.Select the appointment type required.
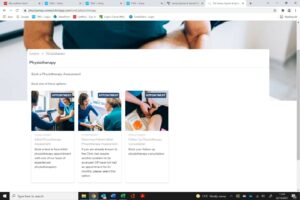
4. You can filter your search by selecting a specific practioner, if you wish to do this it will bring up times and days for this physio only. If you select ‘any practioner’, it will not show the practioner until you click on a day and preferred time (morning, afternoon or evening).
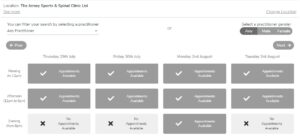
5. Once you have selected your preferred date and time, the available appointment times with the name of the physio will come up as shown below:
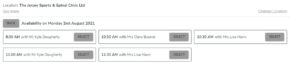
6. Click ‘select’ on your preferred time.
7. The below pop up will appear – please add your preferred mobile number or email address.
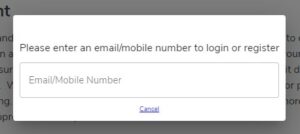
8. Another pop up will appear asking for further registration details, please fill this in and select ‘register’.
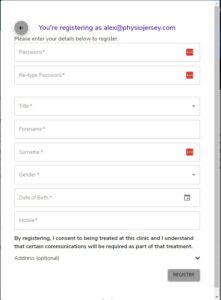
9. The booking will now be held for 10 minutes and to finalize it, you must click the box next to ‘I agree to the terms and conditions and cancellation policy’ and then ‘BOOK NOW’.
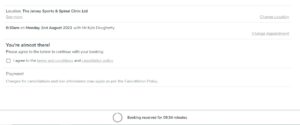
10. The booking is then complete and an email confirmation will be sent momentarily.
How to view or cancel appointment online
First time using our online booking system? Follow these simple steps and get your physiotherapy appointment booked online today!
How to view & cancel an appointment online:
1. Sign into your account (see steps on ‘how to login to your account’)
2. Click on ‘my diary’, on the top tool bar of the account.

3.Your diary will look like the below picture, the dark circled dates in the calendar indicate the dates there is a booked a physio appointment.

If you click on the first purple square for appointments, this will pull up a list of all the appointments made under your account:

4. Select ‘cancel this appointment’ and provide a cancellation reason from the list, if possible. If your reason is not on the list or you do not wish to leave a reason, please click off the drop-down list and select ‘yes’ anyway. You have now successfully cancelled your appointment.
Dummy
How are Goals relevant to my treatment?
You are our valued client, our purpose is to help you feel better and stay better! Our treatments will be focused on helping you achieve your goals, whatever they are. Some clients just want to be able to sleep through the night, some want to be able to walk for longer, enjoy a round of golf, or to manage the stairs pain-free. Meanwhile, others want to summit Kilimanjaro or compete in Ironman events.
Throughout your course of treatment, we will reflect upon the steps achieved and required to help take you towards your goals. Whatever is important to you, is important to us. We will tailor your treatment to help you achieve your goals.
Types of exercise
Your physiotherapist will be able to advise the best type for your condition, but generally:
- Low impact activities such as walking, cycling and exercising in water are good.
- Strengthening exercises working major muscle groups – such as leg raises if you have a bad knee – can help maintain and improve muscle strength to support and protect the affected joint.
- Flexibility exercises that include gentle stretching and balancing may be helpful for mobility.
- Aerobic exercise that increases your heart rate is good for both the heart and lungs as well as staying fit.
- Remember to warm up before a session and cool down afterwards.
Dummy
My massage therapist can “do the physio” so I don’t need to come and see you.
As we explained above, physiotherapy is so much more than just massage. Masseurs have zero training in biomechanics, pain management, advanced exercise prescription. Massage is just one element of the overall treatment plan. Your rehab is likely to be incomplete and temporary, if you only try to massage it away.
Surely I need an MRI scan of my back before having physio?
We understand that it can seem counterintuitive, however, no in most cases, an MRI is not indicated. You will be pleased to know that most back pain settles within three months. Early unwarranted MRI scans are actually associated with higher intervention rates and worse outcomes. MRI scans can give an accurate picture of the spine which can help plan treatment in suspected serious conditions such as cancer, fractures or infections and in very rare cases , cauda equina syndrome.
MRI scans cannot tell how someone feels and are not a diagnosis. The MRI is rarely indicated for back or neck neck pain and should only be organised after an assessment with your physio or GP. Spinal MRIs must be interpreted in the context of the overall clinical assessment and not assessed in isolation. For those with back pain, MRIs frequently report very normal features such as disc degeneration or disc bulges. These findings increase with age and can be a sign of naturally maturing spine.
Nine out of 10 people with no neck pain have disc bulges on MRI, and most people in their 20s have bulging discs. There is good evidence to suggest that unwarranted MRI scans are actually detrimental to patient well-being and lead to poorer outcomes. Let us examine you and together we will decide if an MRI is necessary.
I have “Wear and Tear”, there’s nothing physiotherapy can do to help me, is there?
Osteoarthritis is very common – about 7.4 million people in England over the age of 45 have it. It is fair to say that any one of us over the age of 30 may show some signs of maturity in our tissues. Scans aren’t always needed to diagnose it. It can happen when the joints become damaged with age and injury. Being overweight is another risk factor. Some people have mild symptoms. For others the pain, stiffness and swelling can be severe. That can make exercising difficult, but according to the new NICE guidelines, physical activity should be the main treatment – not painkillers.
However, exercise is the key! Exercise builds muscles and can help people maintain a healthy weight, which is important for managing osteoarthritis. Yes, it may hurt to begin with, but can then ease pain and help individuals with osteoarthritis stay supple, and healthy.
Arthritis charities are concerned that too many patients are put on painkillers rather than getting the right type of help – whether that is exercise therapy or a timely hip or knee replacement. Let’s be honest, there are a backlog of operations due to the pandemic. This means many who need surgery are still waiting and this may take some time to clear. On a positive note, most hip and knee replacements last longer than first thought.
How often will I need to come in for treatment?
There is not a formula for that. It will entirely depend upon your injury or your post-op protocol. Sometimes an intensive burst of appointments is indicated, perhaps 3 times /week but as the treatment progresses, the appointments will be spaced apart more.
Your physiotherapist will outline this with you and the reasons for it. In most cases, a course of treatment is indicated in order for you to be fully recovered and to help keep you injury free.
What's the Difference Physiotherapy, Osteopathy &Chiropractic?
This is a great question and one that we are asked frequently. Each profession may answer it differently. We are actually more similar than different. All three professions are highly regulated, and we must all be registered with the Health Care Professions Council in order to practice.
Each profession also has its own governing body that we adhere to for standards, ethics etc. In broad terms, all three professions approach injury from different perspectives. Chiropractors underpinning beliefs is that the nervous system must work optimally, and they perform adjustments or manipulations to achieve this. This may need to be performed at regular intervals to maintain the condition.
Osteopaths believe that it is a matter of sub-optimal movement in the joints that causes the injury. As such, they too perform techniques to restore movement. Meanwhile, Physiotherapy is a blend of both with an additional beliefs that quality of movement is important, as is strength, and balance too.
Physiotherapists will assess movement, strength, nerve testing, balance testing as well as functional movements (e.g. how you move between sitting to standing or raise your arm overhead). Then we piece all the findings together and bring together a plan that addresses the deficits and addresses your goals. Some colleagues from other professions refer their clients to us for rehab. This cross-referral benefits clients so that any adjustments are then maintained by the body better.
Why should I go to the JSSC for my treatment?
You are most welcome to choose your preferred physiotherapy clinic. Sometimes we can be influenced by your GP or Consultant or indeed by a recommendation from friends or family. You are the patient and it is your choice.
Of course, we think that we are the best physiotherapy clinic for you. We have a team of physiotherapists with a breadth and width of knowledge and experience. We invest heavily in training and most of our staff are working at Masters level qualifications. All of our staff have world-class basics and each member of the team has their additional area of specialty: Alex S&C, Clare for hips, Nigel for headaches/hypermobility, Kyle for end-stage rehab, Lisa for post op, ankles.
Between us, we have nearly 60 years of knowledge and experience. You will not find this in any other physio clinic in Jersey.
We have a purpose-built clinic with excellent rehab facilities to help you recover as fast as biologically possible. We have full admin support to enable your account to be processed with ease.
Since we set up the business in 2007, we have seen the marketplace change in Jersey. Others have followed our methods. This is a great benefit for the client so that we are truly moving towards evidence-based, client-centered care.
Over the years, some staff have left us and set up their own clinics. There is no greater compliment to our clinic and to our profession to see our staff blaze their own trails. We firmly believe that a candle loses nothing by igniting another flame. We genuinely wish them well. We are all motivated to help clients move well.
Dummy
How To Login To Your Account
First time using our online booking system? Follow these simple steps and get your physiotherapy appointment booked online today!
How to login to your account:
1. To login to your account ensure the following web address link is used: https://www.physiojersey.com/
2. At the top right-hand side, you will see an option to ‘book now’ please select this option.

3. Now please click on the ‘login/register’ option on the top right-hand side of the page

4. Enter the email address or mobile number that is registered with the patient profile.
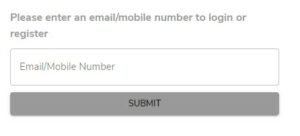
5. Enter the password that was chosen when you first created the online booking account and press enter.
6. You will now be logged in to your account. The top tool bar will now have changed to look like the below:

You can view booked appointments, view availability and can move/cancel appointments if necessary. Please remember that you cannot move or cancel bookings that were made in the clinic by the receptionist, to make any changes to these bookings this will need to be done by the clinic.
How to change your password
First time using our online booking system? Follow these simple steps and get your physiotherapy appointment booked online today!
How to change your password:
If you have forgotten your password, please use this step-by-step guide to reset your password.
1. Try to sign in using steps 1-5 above with ‘how to login to your account’.
2. Once you have entered your password incorrectly three times, the account will be temporarily suspended.
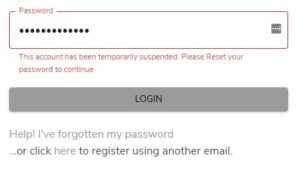
3. Click on ‘Help! I’ve forgotten my password’ and this will send a reset password link to your email address. This email will come from ‘reception@physiojersey.com’ – remember to check your junk folder!
4. The ‘reset your password’ email should look like the below:
![]()
5. Click ‘reset my password’ and this will redirect you to a new tab where you can fill out your new password.
6. Fill out your new password
7. You have now successfully changed your password.
More Questions About Sports Massage?
Click here to get your questions answered.
